Definition of Varicose Veins
Varicose veins are a common medical disease of the leg veins that is most commonly genetically inherited. Varicose veins are abnormally enlarged, swollen, and twisted veins of the legs that have thinned out walls and weakened internal valves. These abnormal blue leg veins can manifest at any point in one’s lifetime, from the teenage years all the way until the golden years. Varicose vein disease afflicts over 25 million men and women in the United States. Varicose veins can occur in anyone, although women are more commonly affected and the disease can often first manifest during or after pregnancy. As people age, forty percent of females and twenty-five percent of males will develop varicose vein disease.
Varicose veins first begin as rather small bulging veins beneath the skin or within the skin, but over time they get larger and more numerous. Once the abnormal veins begin to grow in the leg, they tend to multiply rather quickly. More and more new abnormal vein branches develop in the leg over time, just like a tree grows new branches as time passes. And just like a tree or plant, these abnormal blue bulging veins also enlarge and grow bigger and bulgier as time passes. Soon the leg has multiple areas of worm-like bulging blue veins protruding beneath the skin or within the skin.
Causes of Varicose Veins
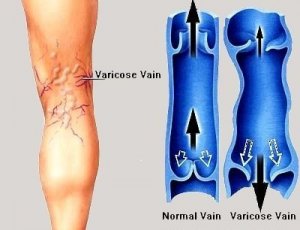
The reason that varicose veins occur is due to the development of faulty vein valves within certain veins of the legs. Each vein of the legs contains a series of many valves that control the direction of blood flow. The normal direction of blood flow in healthy veins is upwards, i.e. towards the heart. Therefore, healthy veins are continuously working against gravity to carry blood to the heart and lungs. But faulty vein valves within varicose veins are weaker than normal and they tend to break and they stop working properly.
The faulty valves then allow blood to reverse direction and travel downwards, i.e. away from the heart and towards the feet. This backward motion or reversal of blood flood is harmful to the leg circulation and is also harmful to the tissues of the leg and feet, particularly harmful to the skin. Gravity pressure build-up in the leg veins and leg tissues eventually leads to a progressive “domino effect” of more and more valves failing. The progressive valve failure wreaks havoc on all of the tissues of the legs and eventually leads to multiple detrimental leg symptoms. This disease process that leads to varicose veins is called venous reflux disease.
Venous Reflux Disease & Varicose Veins
Varicose vein disease never tends to stabilize, but rather always worsens as the year’s pass. This progression is one reason that it is so important to get varicose veins evaluated early before further damage can occur to the leg circulation. The longer that the disease is neglected, the worse the legs appear and the more symptoms that develop. Also, the longer that the vein disease is present the more difficult it is to treat.
The most common genetically faulty veins to become diseased in the legs are known as saphenous veins. These veins are located in both the upper and lower legs. The most common location of varicose vein disease is the inner calf and back of the calf. But varicose vein disease can occur in any location of the leg from the groin all the way down to the foot. Varicose vein disease commonly involves both legs but it can be isolated to a single leg. If one leg is involved, it can be beneficial to have the opposite leg evaluated by venous ultrasound as well to see if the same process is occurring in that leg.
Common Symptoms of Varicose Veins
The most common symptoms of varicose veins of the legs are pain and swelling. Some people seek medical attention due to the unsightly appearance alone. Other commonly described symptoms of varicose veins are itching, burning, heaviness, cramping, throbbing, tiredness or easy fatigue of the legs, and restless legs. Over time, many people suffering with varicose vein disease also develop progressive skin damage of the lower legs, ankles, and feet. This skin damage manifests as brown pigment in the skin, redness of the skin, skin flakiness, hardness or puffiness of the skin, or even skin breakdown with development of ulcers or wounds. This end-stage of the condition is referred to as venous stasis ulceration.
Therapy for Varicose Veins
Therapy for varicose veins will vary depending on the underlying anatomy of your abnormal veins, the size of your veins, and also what your therapeutic goals entail. If you are strictly looking to slow down the worsening of your veins or are only wishing to treat minor symptoms such as mild achiness or swelling, sometimes the use of compression stockings and herbal supplements will be adequate. If your goals are to completely remove the varicose veins and obtain a cure, then the therapy will be interventional treatments by the physician.
The size and severity of you varicose veins will determine what interventional therapies you may be a candidate for. For example, if your physician determines that your veins are too large and extensive to resond to less invasive therapies, then sometime your vein specialist will recommend a surgical procedure to remove the vein. Whereas if you came to see the doctor earlier in the course of your varicose vein disease before it has had time to spread and become severe, then you are much more likely to be a candidate for less invasive procedure that will not require surgical removal of your varicose veins.
Some of the less invasive options (i.e. non-surgical options) for the treatment of varicose veins include ultrasound-guided procedures such as sclerotherapy and Varithena. These procedures involve the injection of liquid medication into the abnormal varicose vein under the guidance of an ultrasound machine. Another example of a less invasive option t0 remove varicose veins is the use of a vein laser or a vein radiofrequency catheter to heat an abnormal vein to cause it to fade and absorb. This procedure is referred to as a thermal ablation. Lastly, newer therapies such as VenaSeal vein glue can also allow a physician to remove varicose veins from the legs without the need for a surgical incision.
Which one of these varicose vein therapies you will be a candidate for will be determined by a physical exam by one of our vein specialists. Sometimes you will be a candidate for more than one treatment option and our physician will explain the various options to you. The good news is that there is always a way to rid your body of these diseased veins! Let our vein specialists come up with a treatment plan that is in tune with your goals and expectations.
Contact Our Vein Center To Assess Your Varicose Veins
If you think that you or someone that you know is suffering from leg vein disease, please contact our Vein Specialists for a consultation. The condition can be successfully treated and cured. We offer the most modern state-of-the-art treatments available. And our vein specialist physician is the most qualified to treat your condition due to his education and training, with board certification as a vascular surgeon and vein specialist.
